Is End-of-Life Planning Age Friendly?
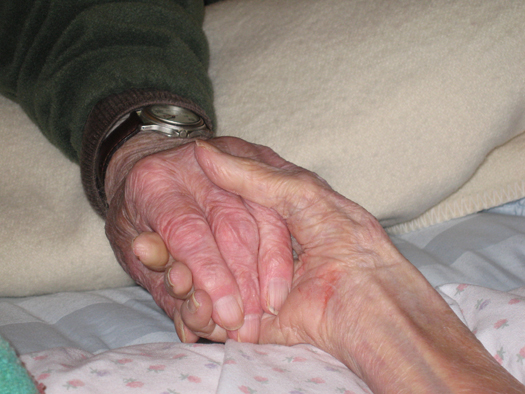
Does end-of-life education belong in an age-friendly community’s effort? Most people don’t use the words “friendly” next to “death” or “dying.” Although, if we agree that we live right up until the moment we die, then it’s natural to include projects in a livable community’s initiative that educate people of all ages on the components of good endings, making choices about care in the last stage of life, and about options for during and after death.
Most people are uncomfortable talking about these topics. The first step is to engage people to talk. Once they begin to share, especially in a group, they usually want more.
My parents made our household a place where we talked pragmatically about illness, dying and death. They gave my brother and me the ultimate gift—they talked candidly about their own wishes, documented them, and made sure we were comfortable following through with their choices.
Rather than being a dinner table topic that seemed morbid, it became natural for us to hear their feelings about the medical procedures that relatives or friends were going through, sprinkled with our folks’ own wishes, smothered in a sauce of humor and irreverence. For example—by the time we were in high school, we knew our parents wanted to be cremated. Dad used to joke he wanted his ashes sprinkled over the 14th hole of his favorite golf course because that’s where he got his “hole in one.” And we hope he meant it, because we did that! And our mom used to say she wanted her headstone to read, “I told you I was sick.” We were used to going to funerals and talking about wills.
My dad also had his own way of giving his “Do Not Resuscitate” orders. When he was 75, we heard this direction: “If you come to visit and see me lying unconscious on the floor, don’t call 911. You don’t know how long I’ve been there. I don’t want to risk being kept alive while brain-dead. Here’s what I want you to do—step over me, sit down, watch your favorite TV show and wait 30 minutes. Then, when I’m good and dead, you can call 911 or whatever you think you have to do.” No questions there.
They clearly documented their plans. And finally, when they were declining, we knew when it was time for hospice rather than healing. They lived to be 95, were married for over 70 years, and died within 30 days of each other. My brother and I had no confusion, arguments, or guilt over what we should do for them and with them. We were able to grieve, and celebrate their lives.

My parents lived until 95 and were married for 70 years.
My effort to tie end-of-life issues to an age-friendly community project comes out of the value I received from my parents by the way they handled these issues. End of life—the operative word being life—is simply another stage, yet it is rarely discussed in city planning. What does the city or county have to do with your dying and death?
Understand—I’m not suggesting that people be required to file a report or make their preferences public. But informed people are happier. Funeral directors see tangible benefits when families and loved ones discuss and put plans in place long before the onset of illness. Just talking about options and plans as outlined by Funeralresources.com can minimize stress, disagreements, and provide peace of mind. If encouraging people to talk about this uncomfortable subject can increase the possibility of having a “good death,” it is worth implementing.
I realize my parents were the exception, as they taught us over years of input, sharing, and asking questions. As a result, I’m now a hospice volunteer and a certified Heartwork facilitator about planning for good endings.
In my volunteer and facilitation work, I show the film “Speaking of Dying” to groups all over the Northwest. I hear about resistance from all sides. Often, when an older adult brings up their will, advance directive, or end-of-life wishes, their loved ones say, “Please let’s not talk about it. You’re nowhere close to dying!” Then, when it’s the children who bring up the topic, imploring their parent to please fill them in on details, the parent often says, “Why bring that up? Are you just waiting for me to die?” When no one is willing to bring it up, families are in conflict, confusion, or both. I have learned that it’s too late to wait until the person is in their last days to have a meaningful discussion. At more than one bedside, I have heard, “I’m not sure I am doing what s/he would have wanted. We never talked about it.”
To engage people in normalizing end-of-life discussions, here are some project ideas for individuals and organizations:
- Implement an Advance Directive initiative—taking our cue from Lacrosse, WI—one city that is leading by example—assuring that every citizen has an Advance Directive in place.
- Educate—create opportunities to educate adults and older adults by placing provocative informational kiosks in numerous locations such as city hall public waiting rooms, VA waiting rooms, hospitals, doctor’s offices, clinics, fire departments, police departments, libraries, parks and recreation locations, community centers, senior centers, and retirement communities.
- Sponsor talks if you don’t like to talk about it. Consider this perspective from an AARP Magazine interview with Jane Fonda in connection with her series, Grace and Frankie:
“The past few years, I’ve made a real point of cozying up to death and making it a friend. That’s what I always do with things that frighten me. I read about death, and I think about myself dying and how I want it to be. It helps me to plan. If you know you want to have certain loved ones around you, then you have to live in a way that will have them there. And you don’t want important things going unsaid before you die. Death is inevitable, so why not make peace with it? I’m not scared of it at all.”
Sponsor talks, such as the Heartwork workshops mentioned above, Death Café’s, and Wisdom Cafes offered by King County Library System’s 50+ Program to help get the conversation started. - Screen the film “Speaking of Dying” throughout the county.
- Provide funding for specific training for medical professionals, hospitals, and clinics in how to talk about palliative care, hospice, the Death with Dignity Act, Voluntary Stopping Eating and Drinking (VSED), and completing an advance directive.
- Partner with individuals and organizations that provide information such as End of Life Washington, People’s Memorial Association, most funeral homes, and Heartwork.
My answer is, “Yes! End-of-life education is an essential component of any age-friendly community’s effort.” With our ever-aging demographic, the majority of us are either reaching the next stage of life or experiencing medical circumstances where this knowledge is power, or we have parents or grandparents who are.
We are all in this together—we are all aging—so why not tackle the topic that has been taboo during the last century? We can give each other the ultimate gift of knowledge and peace.
Resources
1. Speaking of Dying, Trudy James, Executive Producer, 2014 (local film maker)
2. Butler, K. Knocking on Heaven’s Door. Scribner, (2013).
3. Gawande, Atul. Being Mortal: Medicine and What Matters in the End. (2014).
4. Kalanithi, P, and Verghese, A. When Breath Becomes Air. Random House, (2016).
5. Shacter, P. Choosing to Die. (2017).
6. Volandes, A. The Conversation: A Revolutionary Plan for End-of-Life Care. (2015).
7. Federal Law on Advanced Directives
8. End of Life Washington
Contributor Dori Gillam, is an Age-Friendly Communities Task Force member and hospice volunteer who facilitates workshops about planning for good endings. Dori has written a number of excellent articles for AgeWise, including Aging is a Laughing Matter (May 2016) and Why Don’t We Plan for Death and Dying Like We Shop for a Car? (September 2014)
![AgeWise King County [logo]](https://www.agewisekingcounty.org/wp-content/themes/agewisekingcounty/images/logo.png)