They Have My Best Interests at Heart

Philip Culbertson tells of his journey to the diagnosis of dementia and of how his life has changed since accepting his children’s help.
I’d moved back to the United States after retiring from a very gratifying career overseas and had landed a job teaching part-time at the local community college in Palm Desert, California. Late in 2011, while being driven to the college by a student, we were in a car wreck. I was severely concussed. My doctors followed the progress of my brain injury for over three years, but while they could see the physical damage to my brain, what they couldn’t really tell was how much damage was concealed within those x-rays.
During those three years, two different psycho-neurologists and two different psychologists tried to make sense out of my repeated test results. Ultimately, in the fourth year, we gave up. By then it was clear that I’d lost my perspective on what was happening and what would be needed. I cooperated when my kids announced that they were moving me to Seattle in the hopes that a larger city would have more sophisticated testing equipment.
My two children tell me that I was “acting out” long before I myself can remember doing so. Certainly, I was aware that I was being extremely generous with my life savings, thinking that treating myself to new clothes (buying up to 10 shirts at a time for example), pledging funds to political and charitable organizations and taking friends to dinner often, and footing the bill, was just what people who were comfortably retired after a successful career were supposed to do. However, my children were much more frugal, having become aware that as we age, we have more and more expenses to bear. They were right and I was foolish.
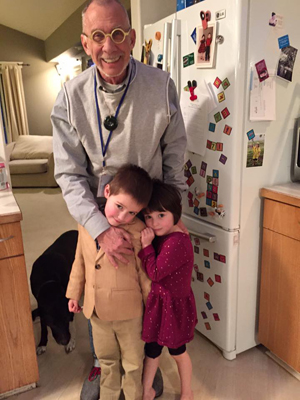
Philip Culbertson enjoys time with his grandchildren.
In late spring 2015, brain x-rays were showing sufficient injury that my children decided to step in and take over large parts of my life. I let them. I’ve heard too many stories over the past several decades to know not to argue with my kids but to hear them out. Most of the time they understood me, probably because we’ve been so close over 30 years. And I have always trusted that, when needed, they would have my best interests at heart — although according to their definition!
While I’m sure it was taxing for them, they persisted on presenting things this way: “Dad, here are three choices that need to be made, and we’d like you to choose the one you feel is best. Then we can all discuss together whether we agree with your choice or not.”
Their strategy has worked so far, for the most part, to everyone’s benefit. In hindsight, that whole phase in which we were involved in a sort of tug-of-war was the most critical phase for me. At that point I let go of my need for control, sensing that my kids now knew better than I did about what was needed.
In early summer 2015, I flew to Seattle to tour possible places to live. We kept in mind that our search was for me—at risk of losing my mind but according to an unknown timetable. My daughter had done her homework well. I didn’t have to see all the sites before I realized how well she knew me. The first place was wonderful and I wanted to move in immediately but she insisted that I at least see the second place.
At both locations, arrangements were made for me to meet some of the residents. I found that, in both groups, each person had experienced some unique brush with death and they had grown to respect, challenge, support, and rescue one another. And importantly, I found that there was a reliable system of professionals and carers, and that no one needed to experience alone the taxing and often frustrating things that mark the end of life.
Shortly after the decision was made to move me to Seattle, both my kids took me to Harborview Medical Center, where we heard the diagnosis: “Early Alzheimer’s—with a life expectancy of two to 20 years.”
The first three to four months in the residential care center were pretty rocky for all of us. I’d been single for years and certainly not used to taking orders from anyone, especially my children. I still wanted to be the parent but I was increasingly unable to make good decisions. That made me angry with them—and with myself!
The more I talked openly with others, the more I learned. Feeling ashamed is one of the great enemies of a healthy approach to Alzheimer’s and dementia. Shame can cause us to hide, stop telling the truth, avoid others, skip attending worship, not enjoy our friends, or fail to take care of our own bodies.
With my kids’ help, I accumulated a bevy of supporters, including a therapist, a hospital chaplain, the doctors at Harborview, various other professionals and specialists and a place to worship. Most importantly, I have my children and grandchildren. Together we are learning that none of us should hide in the dark out of fear, however much each of us also has individual needs to be left alone at times.
I have good days and bad days, and many days are a combination of both. I’ve always slept very well. Now I often don’t. I start into a sentence and then can’t remember what I was going to say. Sometimes I blank out on particular words, or I can’t pull up the names of friends even when they are standing near me. I have learned to write EVERYTHING down, in detail, including things that I was quite sure I’d never forget to do.
The center has taught us the importance of establishing a daily routine, possibly built around the times when we take our medications, and to prioritize our time. For example, I now have many more doctors’ appointments in my life than ever before. No matter how intrusive I feel they are, they must be prioritized over my other commitments and activities.
In the residence where I live, I have been given a one-on-one Alzheimer’s consultant who sees me weekly. She has encouraged me to create a list of the things that I believe are making my life more manageable, most of which are supported by the medical literature. My list for her today was:
- Play the piano, even if my hands are trembling.
- Work crossword puzzles, the more difficult the better.
- Go for a walk—about an hour a day.
- Play with my grandchildren when they visit.
- Sing weekly in a men’s barbershop chorus.
- Maintain a part-time job—in my case as an editor of academic articles for publication.
- Teach a course to a group of residents on Third Century Jewish literature.
- Make sure my spiritual needs are being met on a regular basis by people whom I trust.
My journey through Alzheimer’s continues to be marked with alternating times of bravery and fear, expectation and resignation, clarity alternating with frustrating confusion, and one hell of a lot of paradox. Yet journeys like mine need to be brought into the open rather than kept in the dark, addressed rather than being ignored or minimized. By sharing our story, I believe the fear of death is challenged and ultimately even transformed.
Contributor Philip Culbertson wrote this article for Tui Motu, where it appeared in June 2016. It is reprinted here with his permission.
![AgeWise King County [logo]](https://www.agewisekingcounty.org/wp-content/themes/agewisekingcounty/images/logo.png)